In a small rural clinic in the Philippines, a mother named Jhoyme sits on an examination table, anxious and excited. At 33, she is expecting her third child – but for the first time ever, she’s about to see her baby.
As the community midwife passes a handheld ultrasound probe over Jhoyme’s belly, a grainy black-and-white image appears on a portable screen . “Malaki pong tulong ito sa amin… we can see the baby’s gender, hear the heartbeat, and monitor growth,” Jhoyme says with a smile . For her and countless women in remote villages, prenatal ultrasound has long been a luxury out of reach – requiring travel to distant hospitals and costs they cannot afford . Now, that is starting to change.

Bridging the Gap in Rural Maternal Care
The Philippines faces a persistent challenge in maternal health. Thirteen mothers die every day from pregnancy-related complications, according to a UNICEF report . The country has one of the highest maternal mortality rates in Asia – well over 100 deaths per 100,000 live births as of the late 2010s – with rural areas disproportionately affected . (By comparison, the rate in 2020 had improved to about 78 per 100,000 , still far above global targets.) Most of these deaths are preventable. The World Health Organization emphasizes that “all women need access to high quality care in pregnancy, and during and after childbirth” . Yet in many isolated Philippine communities, women often receive only basic prenatal services like blood pressure checks and vitamins – if they see a healthcare provider at all . Key obstetric complications frequently go undetected until it’s too late. Others only learn about life-threatening issues during labor itself, when options are limited .
This is tragic, because many of the deadliest complications can be spotted months earlier with a simple ultrasound scan. Up to this day, the major causes of maternal deaths – severe hemorrhage (often from abnormal placental attachment), obstructed labor (for example, a baby in breech position), undiagnosed twins – are all conditions that ultrasound can easily detect by mid-pregnancy . In fact, the WHO recommends at least one ultrasound before 24 weeks’ gestation for every pregnant woman . In remote Philippine provinces, however, that recommendation has gone unmet due to a lack of equipment and specialists. Many rural health units have no sonographer or doctor trained in obstetric ultrasound, and villagers would have to travel hours (by boat, bus, or foot) to reach a hospital in the nearest city . For poor farming and fishing communities, the cost and distance mean skipping scans altogether. As Dr. Steffan Haller – a radiologist working to improve maternal care – observed, in some areas “one doctor serves tens of thousands of people”, making routine prenatal imaging nearly impossible .

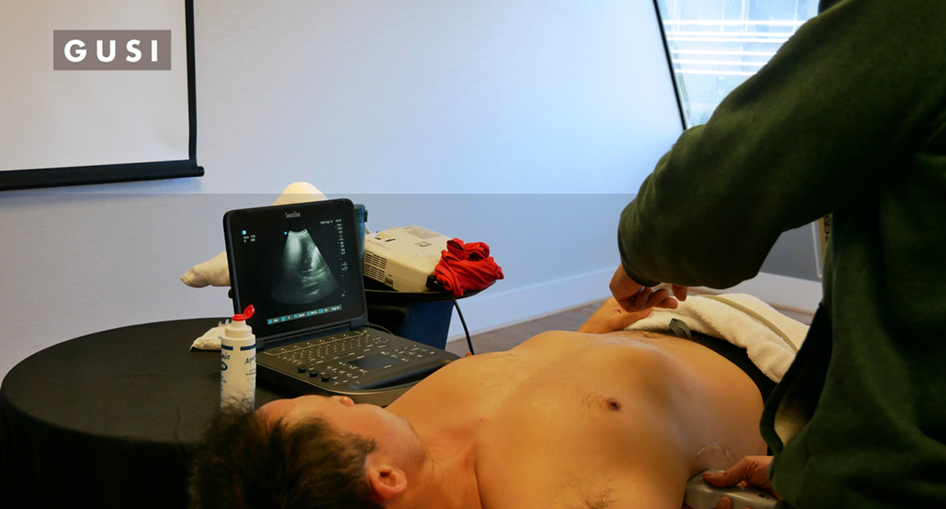
Enter the era of handheld, point-of-care ultrasound (POCUS) devices. These are portable ultrasound probes that pair with a smartphone or tablet, bringing the power of imaging to practically anywhere. Instead of a bulky machine in a distant hospital, a pocket-sized device can be carried into a village by a midwife or local doctor. With basic training, frontline health workers can use them to check on pregnancies during regular prenatal visits. The goal is simple: find problems early, intervene early. If a scan at 6 months shows a low-lying placenta (which could cause dangerous bleeding in delivery), the mother can be referred to a provincial hospital well before she goes into labor. If a baby is in a transverse or breech position, a plan can be made for a safe delivery (or even an attempted repositioning) rather than facing an obstructed labor at home. This early warning and preparedness can literally save lives of both mother and child.
A healthcare professional in the Philippines holds a handheld ultrasound probe connected to a tablet, demonstrating the portability of modern point-of-care ultrasound technology.
Point-of-Care Ultrasound: A Game Changer on the Frontlines
The introduction of portable ultrasound in rural healthcare is transforming maternal health outcomes. Community health workers and nurses, once armed with only stethoscopes and blood pressure cuffs, can now “see” inside the womb. Training local providers in basic obstetric ultrasound has proven feasible and effective. Studies confirm that even with limited training, midwives and general practitioners can perform quality scans in their clinics . In one Philippine program, for example, community healthcare workers were taught to scan for five key obstetric factors – fetal heartbeat and number of babies, placental location, fetal presentation (position), and amniotic fluid volume . The results were encouraging: the trainees’ interpretations of the ultrasound images agreed with expert supervisors about 95% of the time . The handheld devices themselves were also highly reliable, with scans closely matching the image quality of standard hospital machines . This means a rural nurse with a few days of ultrasound training can detect most of the same red-flag conditions that an OB-GYN could, right at the point of care.
Early detection is only half the battle – but it makes a huge difference. If you know a complication is coming, you can prepare for it. A recent scoping review of antenatal ultrasound initiatives across Asia, Africa, and Latin America found universally positive outcomes: introducing point-of-care ultrasound led to higher antenatal clinic attendance and lower maternal and neonatal mortality rates in those communities . Crucially, the review noted that local healthcare workers were successfully taught to perform the scans with short training courses, showing that task-shifting this skill to frontline providers is workable .
Indeed, bringing ultrasound to the community can set off a virtuous cycle. Pregnant women become more motivated to attend prenatal visits when they know they can see their baby and get a proper check-up – no longer just a routine blood pressure and weight, but a memorable bonding experience and reassurance of the baby’s health. Providers, in turn, gain confidence and data to guide care. “Before, midwives had no way of knowing the mother and baby’s condition,” one Filipina midwife explained. “Pero ngayon… mas maipapaliwanag na namin ang komplikasyon at pangangailangan gamit ang ultrasound” – “but now, we can better explain any complications and what interventions are needed, using the ultrasound” . This builds trust in the healthcare system and encourages women to deliver in health facilities if risks are identified. In the Philippine context, many complications like placenta previa or twins necessitate delivering at a hospital with surgical capability. Thanks to point-of-care scans, rural clinicians can flag those cases early and arrange referrals to higher-level hospitals weeks in advance . Operating these portable scanners in village clinics thus helps ensure high-risk pregnancies are managed in the proper setting .
The impact of such initiatives is already evident. In one pilot project in the Philippines, 31.7% of pregnant women scanned were found to have an unsuspected issue, such as abnormal placentation or a malpositioned fetus . By averting home deliveries in those high-risk cases and getting mothers to appropriate care, researchers estimated that the ultrasound screenings “could have possibly averted” about 6.3% of maternal deaths and 14.6% of neonatal deaths in that population . In real terms, that means babies born safe and mothers surviving who might otherwise have faced life-threatening complications. Moreover, nearly all the women who were identified with problems in that program went on to deliver in hospitals or birthing centers (93%), rather than at home, showing a clear shift toward safer delivery practices . As another example, a Filipino OB-GYN, Dr. Marilou de Vera, has recounted how during two-day outreach missions with a handheld unit, her team can now screen 200 to 450 pregnant women – women who line up at a rural health post for a free ultrasound that was never available to them before . Each one of those scans is an opportunity to catch a complication in time or simply to give an expectant mother the assurance that her pregnancy is on track.
The evidence is overwhelming: what was once a missing piece in rural maternal care – diagnostic imaging – can be brought to the frontlines, with profound effects. As a news feature on one such project declared, “the results speak for themselves.” Women who used to go through pregnancy essentially “blind,” hoping for the best, are now receiving critical prenatal care at no cost, in their own communities . Most maternal deaths are preventable, and point-of-care ultrasound is proving to be a potent tool in the prevention arsenal.
ScanOne and ScanHub: Empowering Healthcare Workers with Technology
As part of this transformative shift, ScanOne and ScanHub are playing an integral role in ensuring that healthcare workers have the tools and support they need. ScanOne, a user-friendly ultrasound solution, empowers community health workers to perform and interpret ultrasound scans quickly and effectively. In rural areas where healthcare providers may lack extensive training, ScanOne offers simplified functionality, ensuring that even the most basic scans are accessible. The device connects seamlessly with mobile devices, enabling health workers to conduct ultrasound exams with minimal complexity.
ScanHub, a comprehensive healthcare platform, supports this initiative by centralizing scan data, allowing healthcare providers to share results with specialists remotely. This system enables real-time consultations and second opinions, giving clinicians in rural areas access to expert guidance without the need for travel. ScanHub allows for ongoing patient monitoring, ensuring continuity of care even after the ultrasound scan. Together, ScanOne and ScanHub create a robust, scalable solution for improving maternal and neonatal health in remote areas. These tools are making it easier for local healthcare workers to deliver high-quality care, improving outcomes for both mothers and their newborns.
Training Community Heroes in Catanduanes
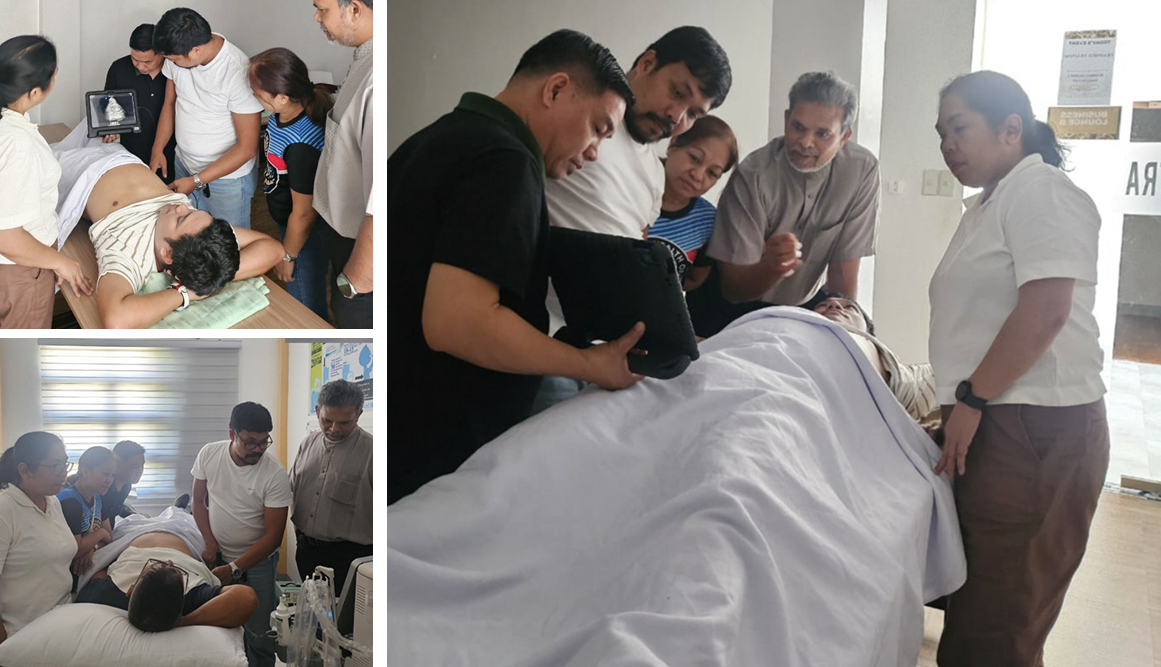
Recognizing these benefits, organizations and health authorities are scaling up ultrasound access in underserved areas of the Philippines. A shining example comes from the island province of Catanduanes – a mostly rural, coastal province often called “The Land of the Howling Winds” for its remote location and frequent typhoons. In May 2025, a landmark initiative was launched to build local ultrasound capacity here. The Global Ultrasound Institute (GUSI) conducted its first-ever in-person point-of-care ultrasound course in the Philippines, held in Virac (the capital of Catanduanes) . The three-day intensive training brought together municipal doctors and nurses from Virac, Viga, Gigmoto, and San Miguel, four of the small towns on the island . These healthcare providers usually operate with minimal resources, often serving as the first and only line of care for far-flung communities. For them, learning ultrasound isn’t just a new skill – it’s a lifeline for their patients.
🩺 Led by Dr. Shaik Farid Abdull Wahab, an experienced emergency physician and POCUS educator, the course focused on real-world ultrasound skills for primary care . Over the training, participants rotated through hands-on stations, practicing scans on volunteer patients and simulators. They learned to assess the lungs (vital in a country with a high burden of tuberculosis and pneumonia), the heart (for signs of heart failure or fluid around the heart), the abdomen (to spot internal bleeding or organ abnormalities), and of course obstetrics – scanning pregnant women to determine gestational age, fetal position, placental placement, and more . By the end of the workshop, a local nurse could confidently perform an ultrasound exam to check a pregnant mother’s baby and a rural doctor could use the device to help diagnose why a patient was short of breath. One of the organizers noted that the training was “immersive, hands-on” and tailored to “frontline care” needs – exactly the scenarios these providers face daily in their community health centers.
Importantly, the Catanduanes course was a collaborative effort. It was run in partnership with a philanthropic team from Traditional Medicinals, an organization committed to supporting community health initiatives . The program also received modern handheld ultrasound devices from Butterfly Network, Inc., ensuring that each trainee had a state-of-the-art scanner to practice with. Armed with these Butterfly devices – which connect to a smartphone and display ultrasound images via an app – the trainees could immediately apply what they learned in a real clinical setting. “We’re honored to help bring frontline ultrasound education to more communities,” GUSI announced after the successful completion of the course, highlighting how such partnerships make it possible to reach remote areas.
The training in Catanduanes did not end with just a one-off workshop. In collaboration with local health authorities and sponsors, GUSI also launched the “Catanduanes Ultrasound Fellowship” – a novel initiative to provide ongoing mentorship and support for the graduates of the course . This fellowship means that over the coming months, the newly trained doctors and nurses will receive case reviews, tele-ultrasound supervision, and continuous education to solidify their skills. Such follow-up is crucial: it ensures that the ultrasound machines don’t just gather dust in a cabinet, and that the providers gain confidence through experience. It also helps build a sustainable culture of ultrasound use on the island. In a sense, a local network of ultrasound champions is being cultivated, who can in turn train their colleagues and advocate for broader use of POCUS in community health.
A Collaborative Path Forward
What is happening in Catanduanes is part of a larger movement to advance maternal and neonatal health in the Philippines through innovation and community empowerment. From the mountains of Luzon to the islands of the Visayas and Mindanao, portable ultrasound technology is reaching communities that once had no access to such diagnostics. Nonprofit organizations like Life Matters International (led by Dr. Haller) have been training midwives in provinces like Occidental Mindoro and Palawan to use POCUS devices in daily prenatal clinics . Government and academic programs are studying the best ways to roll out portable ultrasound in rural health units nationwide . The common thread is the understanding that healthcare workers closest to the community can do so much more when given the right tools and training. As one rural midwife put it, “dati, hindi alam… pero ngayon nagagawa na namin dito” – before, we didn’t know what was going on inside a pregnant mother, but now we can do it here in our clinic .
For global health donors and supporters, these successes highlight a high-impact opportunity. Investing in point-of-care ultrasound for rural maternal health yields tangible, life-saving results. A single handheld ultrasound device – which can cost a fraction of a traditional machine – used by a trained community health worker can serve hundreds of pregnancies per year, detecting which ones need advanced care. The model is scalable and cost-effective: donate devices, train local providers, integrate ultrasound screening into existing antenatal care, and watch the indicators improve. Antenatal visit compliance goes up , emergency complications go down , and most importantly, mothers and babies survive and thrive where previously tragedies struck in silence.
The Philippines is demonstrating how innovation and education can bridge the urban-rural health divide. Combining modern technology (like Butterfly’s and Philips’ portable ultrasounds) with grassroots capacity building (training midwives, nurses, and doctors on-site) creates a powerful synergy. It exemplifies the ethos of “healthcare equity” – making sure that a woman in a fishing village on Catanduanes has the same chance for a safe delivery as a woman in Manila. Each successful ultrasound training or donation not only equips healthcare workers with a new skill, but also sends a message to the community that “we care about you and your baby’s health.” That builds trust, which in turn encourages more women to seek care, completing the feedback loop of improvement.
As we look ahead, scaling up these efforts will require sustained collaboration. The recent Catanduanes course was supported by a tea company’s social responsibility arm, an international ultrasound institute, and local health officials – an example of the multi-stakeholder partnership needed for impact. Global health donors can amplify this by providing funding for more devices and trainings in other underserved regions. The Department of Health and local governments in the Philippines can integrate POCUS training into their regular programs for rural health workers, ensuring long-term continuity. And further research and monitoring can quantify the outcomes – as early data has done – to continually refine the approach.
In the end, the vision is clear: no mother should die giving life, simply because she lives far from a hospital. By empowering community health workers with ultrasound skills, even the most remote barangays can identify risks early and connect mothers to the care they need. The once stark gap between rural and urban maternal healthcare is beginning to narrow. Jhoyme, the mom who saw her unborn child on the clinic screen for the first time, is one of many who now have knowledge and hope on their side. “Most maternal deaths are preventable,” the WHO reminds us – and in the Philippines’ rural heartlands, the prevention is happening, one handheld scan at a time. The sound of a tiny heartbeat on an ultrasound speaker, echoing in a remote village, is proof that change is arriving – and with continued support, it will only grow louder.


