Tuberculosis (TB) continues to be the world’s leading infectious killer, claiming 1.25 million lives in 2024 and affecting over 10.8 million people worldwide. Among the greatest challenges in TB control is timely diagnosis—especially in rural or under-resourced communities where access to X-rays or laboratories can be hours, even days, away.
In a compelling webinar hosted by the Global Ultrasound Institute (GUSI) on June 18, 2025, Dr. Bruno Vargas, a frontline physician from Compañeros en Salud / Partners in Health Mexico, shared invaluable insights into how point-of-care ultrasound (POCUS) is reshaping TB diagnosis in real-time. This post explores his perspectives on lung ultrasound for TB, its potential, its pitfalls, and the emerging technologies like ScanOne and ScanHub that are helping clinicians “pick up the probe” with confidence.
POCUS: A Lifesaving Diagnostic Bridge in Remote TB Care
From the rugged clinics of Chiapas, Mexico, Dr. Vargas has seen firsthand how a handheld ultrasound device can act as a “lifesaving extension of the physical examination.” In places where patients must travel for hours on foot or by vehicle to reach the nearest chest X-ray, the ability to scan at the bedside is transformative.
In multiple cases, lung ultrasound (LUS) revealed TB-related findings—like pericardial effusion or pleural irregularities—prompting program officers to initiate treatment before sputum results even came back. The takeaway? POCUS isn’t about replacing X-rays. It’s about making sure patients don’t fall through the cracks while waiting for them.
“It’s not about replacing X-rays—it’s about getting patients diagnosed and treated when access is a barrier.” – Dr. Bruno Vargas
POCUS: A Lifesaving Diagnostic Bridge in Remote TB Care
The webinar panel, including experts from six countries, acknowledged both the exciting potential and real-world limitations of lung ultrasound in TB care.
✅ The Promise:
LUS is highly sensitive for detecting subpleural nodules, consolidations, and pleural abnormalities—common signs in pulmonary TB.
Studies report 56–100% sensitivity in identifying these findings in TB patients.
LUS can even detect peripheral lesions that chest X-rays might miss.
It enables faster triage—supporting decisions on isolation or treatment initiation even before lab confirmation.
⚠️ The Limitations:
Specificity is low: Many TB-like signs (e.g., consolidations) also occur in pneumonia, cancer, or embolism.
Deep lung cavities—a classic TB hallmark—are usually invisible to ultrasound.
There’s currently no universal criteria for a “TB-positive” ultrasound.
A negative scan doesn’t rule out TB, and a positive one doesn’t confirm it—clinical context remains essential.
Dr. Vargas emphasized that proper training and pattern recognition are key to avoiding false positives and building trust in POCUS as a diagnostic ally.
"Pick Up the Probe": Practice, Train, Repeat
ScanOne and ScanHub: The Tech Tools Behind TB POCUS
Enter ScanOne and ScanHub, digital platforms developed by GUSI that support POCUS from image capture to collaborative learning.
ScanOne (Mobile App):
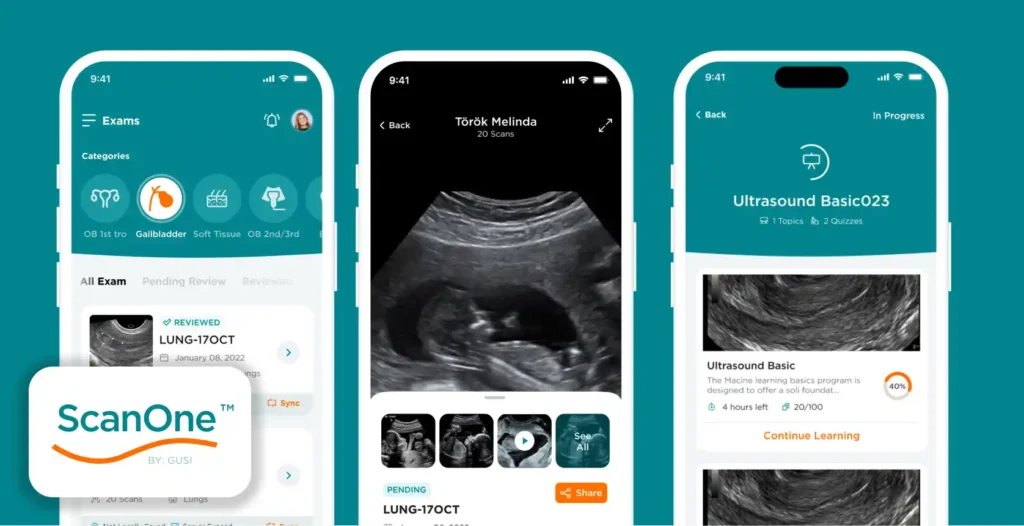
Enter ScanOne and ScanHub, digital platforms developed by GUSI that support POCUS from image capture to collaborative learning.
Acts as a personal ultrasound assistant.
Allows clinicians to securely upload images and videos from handheld ultrasound devices (e.g., Butterfly iQ).
Recent upgrades include Bulk Upload, saving time for busy frontline workers scanning dozens of patients per week.
ScanHub (Cloud Platform):
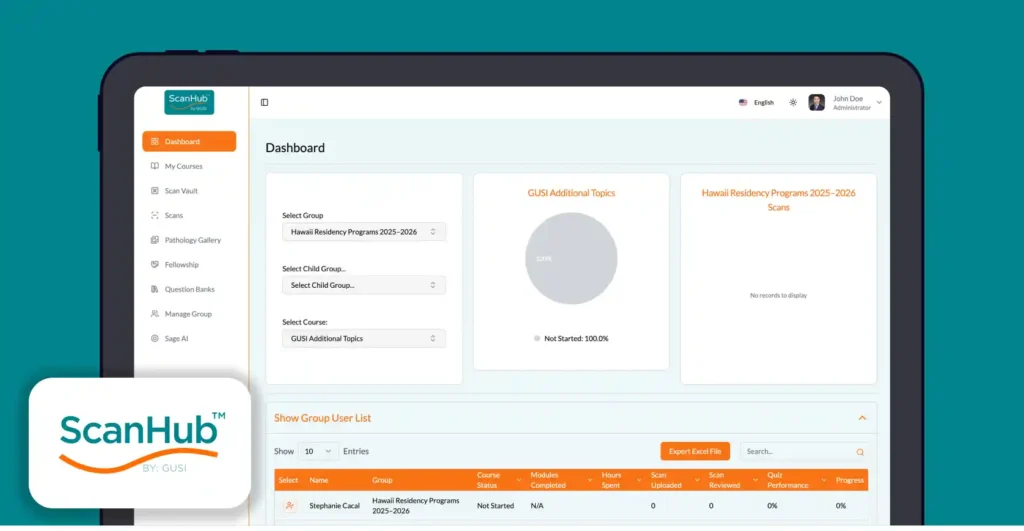
A centralized dashboard for managing, reviewing, and analyzing uploaded scans.
Enables remote consultation, AI analysis, and structured feedback.
Each clinician has a scan portfolio, helping them track progress and receive ongoing mentorship from experts or AI.
These platforms aren’t just improving efficiency—they’re shaping a global learning network and building a data vault of TB-related lung scans that fuel research, training, and AI development.
The AI Frontier: Smarter, Faster TB Insights
AI is beginning to augment TB diagnosis with POCUS. During the webinar, GUSI shared data from recent studies in West Africa showing that AI-assisted ultrasound can reach WHO-recommended accuracy levels for TB detection.
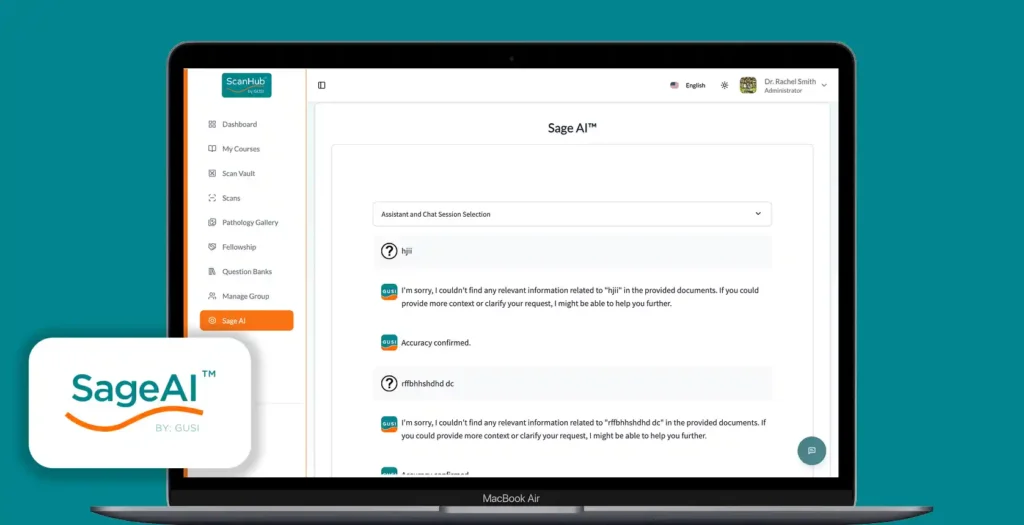
With tools like SageAI™, even newly trained users can get real-time assistance interpreting scans. AI can highlight findings like pleural effusions or B-lines, giving providers a second opinion at the point of care.
Still, Dr. Vargas warned: “AI can’t be a black box.” Transparency, training, and clinical judgment must guide how AI is used.
Looking Forward: Scaling a TB-Free Future, One Scan at a Time
Dr. Vargas’s experience proves that innovation and dedication can overcome diagnostic barriers. Lung ultrasound won’t replace conventional tools, but it’s an invaluable supplement—especially where access is limited.
What’s needed now:
More training for frontline providers
Standardized TB criteria for LUS
More research into diagnostic patterns
More collaboration between clinics, researchers, and tech platforms
Missed the Webinar? Watch It On-Demand
If you want to hear Dr. Vargas’s stories firsthand and explore real-world LUS cases, the full recording of the June 18 webinar is now available online. It’s a must-watch for anyone interested in ultrasound, global health, or infectious disease care.
And keep an eye out—GUSI will be announcing its next global webinar soon.


