Kenya is at the forefront of a point-of-care ultrasound (POCUS) revolution. In rural clinics that once lacked basic imaging, healthcare workers are now using handheld ultrasound probes connected to smartphones or tablets to peer inside the body in real time. Through a collaboration between AMPATH Kenya, the Butterfly Network, the Bill & Melinda Gates Foundation, and the Global Ultrasound Institute (GUSI), two innovative tools – ScanOne and ScanHub – are strengthening diagnostic capabilities, training local clinicians, and improving maternal, fetal, and general health outcomes in Kenyan communities. This blog post explores what ScanOne and ScanHub are, how they function and are deployed in the field, and the profound impact they are having on healthcare delivery in Kenya.
The Need: Bridging a Diagnostic Gap in Kenya

In low-resource settings like Kenya, access to diagnostic imaging has historically been very limited, especially in rural areas[1]. Clinicians have had to rely on physical exams and patient history alone, which often isn’t sufficient to catch complex conditions like pregnancy complications, heart failure, or early-stage cancers[1]. This diagnostic gap has dire consequences: roughly 94% of maternal deaths and the vast majority of newborn deaths occur in low- and middle-income countries[2]. Every year in sub-Saharan Africa, an estimated 200,000 mothers and 28 of every 1,000 infants die during childbirth[3][4] – many from conditions that could be detected and managed if ultrasound were available. In fact, researchers have estimated that fetal deaths decline by about 20% after ultrasound is introduced into antenatal care[5].Recognizing these staggering figures, Kenyan and international partners have prioritized bringing POCUS technology to the frontlines. Midwives and nurses in rural clinics are being empowered with portable ultrasound devices to perform quick, life-saving scans at the bedside. The goal is to catch high-risk conditions early – before they turn into tragedies. As Dr. Kevin Bergman (co-founder of GUSI) noted, “Nearly 95% of maternal and neonatal deaths occur in regions where access to healthcare is limited,” but POCUS can help bridge that gap by making diagnosis faster, easier, and more accurate wherever patients are[3][6].
What Are ScanOne and ScanHub?

ScanOne and ScanHub are the technical keystones of this ultrasound expansion, providing the digital infrastructure to support POCUS deployment and training. Developed by the Global Ultrasound Institute, ScanOne is a cloud-based mobile application (available for iOS and Android) designed for healthcare professionals to securely upload and manage ultrasound images and videos for diagnostic and educational purposes[7]. In practice, a nurse or clinical officer in the field can use ScanOne on a smartphone or tablet to record ultrasound clips and still images from a handheld scanner, then store them in the cloud with just a few taps. All data is encrypted and stored securely.
ScanHub is the complementary web platform – essentially a centralized online hub for ultrasound scans. Through ScanHub (now integrated into GUSI’s “UpScan” platform), clinicians and their mentors can log in to review uploaded scans, provide feedback, and track progress. ScanHub acts as a digital archive and collaboration space: an expert in Nairobi or even overseas can remotely evaluate a scan taken that morning in rural Bungoma county, then share guidance within minutes. GUSI’s platform even integrates an AI-based assistant called SageAI, which offers 24/7 support by answering POCUS questions or helping analyze images[8]. In the near future, such AI tools will be directly incorporated to assist with identifying key findings – for example, software algorithms are being developed to automatically recognize pregnancy risk factors on these scans[9].In summary, ScanOne and ScanHub create a connected POCUS ecosystem: frontline providers capture ultrasound data with the ScanOne app, and those images are synced to ScanHub, where supervisors, specialists, or teaching faculty can perform real-time scan reviews and mentorship[10]. This feedback loop ensures that even after an initial training course, every nurse or midwife has continuing support to interpret scans correctly and improve their technique. It’s a high-tech solution tailored for low-resource settings – leveraging cloud connectivity and smartphones, which are increasingly available even in remote areas, to deliver quality ultrasound diagnostics anywhere.
Collaboration in Action: AMPATH, Butterfly Network, and Gates Foundation





Bringing POCUS and the ScanOne/ScanHub platform to Kenya has been a team effort, uniting clinical, technological, and funding partners:
- AMPATH Kenya – a partnership led by Moi University and North American academic centers – is spearheading on-the-ground implementation. In late 2024, AMPATH launched a four-year initiative to integrate POCUS into primary care across six counties in western Kenya[11]. This program is establishing regional “POCUS Innovation Centers” at county hospitals, which serve as training hubs and ongoing support centers for surrounding health facilities[12][13]. AMPATH provides the local leadership, infrastructure, and healthcare workforce to make POCUS a routine part of care.
- Global Ultrasound Institute (GUSI) – through its UpScan suite (ScanOne and ScanHub) – delivers the training curriculum, mentorship, and technology platform. GUSI educators have worked closely with Kenyan experts to run training workshops and develop protocols. They also maintain the ScanHub cloud system that enables continuous supervision. “We build lasting systems of diagnostic care by working directly with local institutions, training frontline providers, and tracking real-time impact,” explains Dr. Mena Ramos, GUSI’s co-founder[14][15]. GUSI’s role ensures that the project is not just about donating devices, but about building a sustainable ecosystem of skilled users.
- Butterfly Network, Inc. contributes the ultrasound hardware and related software. Butterfly’s iQ+ is a pocket-sized, single-probe ultrasound device that can scan the whole body. Uniquely, it uses a semiconductor “ultrasound-on-chip” rather than traditional piezoelectric crystals, dramatically shrinking cost and size while maintaining imaging quality[16]. This innovation made it feasible to deploy 1,000 such probes for widespread use in Kenya and South Africa under this program[17][18]. Butterfly also helped develop tailored obstetric POCUS training content and continues to refine the technology for low-resource environments (including exploring battery-operated usage and durable designs for the field).
- Bill & Melinda Gates Foundation (and other donors) have provided crucial funding and strategic support. A $5+ million grant from the Gates Foundation kick-started the procurement of 1,000 Butterfly devices and the training of over 1,000 healthcare workers in Kenya and South Africa[17]. In Western Kenya, a new $6.5 million grant (channeled through Panorama Global) is supporting AMPATH’s POCUS scale-up, with funding from Gates as well as partners like Novartis, Eli Lilly, and Merck for Mothers[11]. This philanthropic investment is what allowed the collaboration to reach such scale. The Gates Foundation in particular has been vocal about ultrasound’s potential to save mothers and babies, and has funded both technology development and implementation research in this arena[19][20].
Together, these partners have created a model that combines cutting-edge technology, training, and health system integration. It’s a model that is locally led – working within Kenya’s Ministry of Health structure – but draws on global resources. As Dr. Bergman of GUSI put it, “Point-of-care ultrasound is the stethoscope of the 21st century… it breaks down barriers for patients to receive higher quality care” by bringing imaging to the bedside[21][22].
Training the Frontline: How ScanOne and ScanHub Are Deployed
The deployment of ScanOne/ScanHub in Kenya revolves around training the trainers and empowering frontline clinicians. It began with high-volume training events to build a critical mass of skilled ultrasound users, and now focuses on ongoing mentorship through the platform:
- Intensive Workshops: In the initial phase, large cohorts of midwives, nurses, and clinical officers underwent in-person training. For example, in September 2022 a week-long workshop at Kenyatta University in Nairobi trained 514 providers from 8 counties, chosen from regions with the highest maternal mortality rates[23][24]. By the end of 2022, these graduates were deploying Butterfly iQ+ devices to 224 public health facilities across Kenya[25] – meaning nearly 224 clinics or maternity units now had POCUS capability where it hadn’t existed before. Training covered hands-on scanning techniques and recognizing key obstetric findings: checking fetal heartbeat and growth, identifying multiple gestations (twins/triplets), detecting malpresentation (e.g. breech babies), assessing amniotic fluid, and locating the placenta[26][27]. Notably, the curriculum first created a cadre of about 50 Kenyan sonographers and doctors as local instructors, who then taught the subsequent cohorts[28]. This “train-the-trainer” approach built local capacity and reduced dependency on foreign experts.
- POCUS Innovation Centers: Under the new AMPATH-led phase (launched in January 2025), training is being decentralized. The Webuye County Hospital in Bungoma became the first of six POCUS Innovation Centers, hosting an inaugural class of 24 healthcare workers in January 2025[12]. These centers will each support several surrounding facilities. After the initial 24 “champions” were trained in Bungoma, they assisted in rolling out ten follow-up trainings at sub-county level, reaching 670 additional healthcare workers in that county[12]. Similar waves of training are planned for five other counties in Western Kenya. In total, 4,000 frontline providers (nurses, midwives, clinical officers, and doctors) will gain POCUS skills through this project[13] – an ambitious human-capacity boost. Alongside training, 190 Butterfly probes were distributed to rural health facilities in the first county alone[29], and more will be deployed as training expands. Each site is typically given a Butterfly iQ device (which can plug into a smartphone/tablet) and a tablet preloaded with the Butterfly software and GUSI’s ScanOne app. This hardware+software package essentially turns even a remote dispensary into a miniature imaging center.
- ScanOne/ScanHub for Mentorship: After providers return to their clinics with new skills and equipment, the real work is ensuring they continue to use ultrasound effectively. This is where ScanHub’s continuous mentorship model shines. Trainees are encouraged to perform scans during routine antenatal visits or patient assessments and upload a selection of images or clips via the ScanOne app to the cloud. A team of experienced sonographers and physicians – including Kenyan specialists and GUSI’s international faculty – then review these scans asynchronously on ScanHub. They provide feedback within the platform, noting if the image quality is acceptable, if the measurements seem accurate, or if the case warrants referral. GUSI describes this as providing “real-time feedback, mentorship, and scan review via our platform – ensuring quality, confidence, and continuity” for providers on the frontline[10]. In practical terms, a midwife in a village health center can get guidance on whether that fetal ultrasound shows a placenta previa or not from a senior radiologist many miles away, usually the same day. This safety net builds confidence among the new users. It also allows the program managers to monitor utilization: the platform logs each scan, which helps track how often each site is scanning and what they are finding. (In fact, by monitoring ScanHub data or Butterfly cloud analytics, the team can identify if any clinic has stopped using their device and may need a refresher or troubleshooting visit.)
- Quality Assurance and Certification: The combination of ScanHub mentorship and periodic in-person supervision visits helps assure quality. Trainees must typically complete a certain number of supervised scans to be deemed fully competent. In the 2022 cohort, for instance, providers took a practical exam after the week-long course – impressively, 99% passed a competency exam covering obstetric POCUS knowledge and skills[30]. The high pass rate speaks to the effectiveness of the training. But more importantly, 95% of those providers continued to use POCUS regularly in their practice (adoption rate)[31], which is a testament to how well-integrated the mentorship and support structure (including ScanHub) kept them engaged. One Kenyan nurse, Ms. Sheila Ayesa Masheti – who became a GUSI project coordinator – observed firsthand that “wherever POCUS technology is used by midwives, clinical personnel, and other frontline professionals, it helps improve maternal and neonatal outcomes” by enabling timely, accurate diagnoses[32]. ScanOne and ScanHub are the tools making sure those frontline professionals can perform scans correctly and get a second opinion when needed.
Healthcare workers in Kenya practice with new handheld ultrasound devices during a training session led by GUSI and AMPATH[12][33]. ScanOne (mobile app) and ScanHub (cloud platform) allow these trainees to continue receiving mentorship on their scans even after the classroom training, by securely uploading images for remote
Strengthening Diagnostic Capabilities and Health Outcomes
The impact of these efforts is already visible in Kenyan healthcare facilities. Diagnostic capabilities have been transformed: conditions that were previously detected too late (or not at all) are now being caught early during routine visits. The result is better clinical decision-making and improved patient outcomes across maternal, fetal, and general health domains.
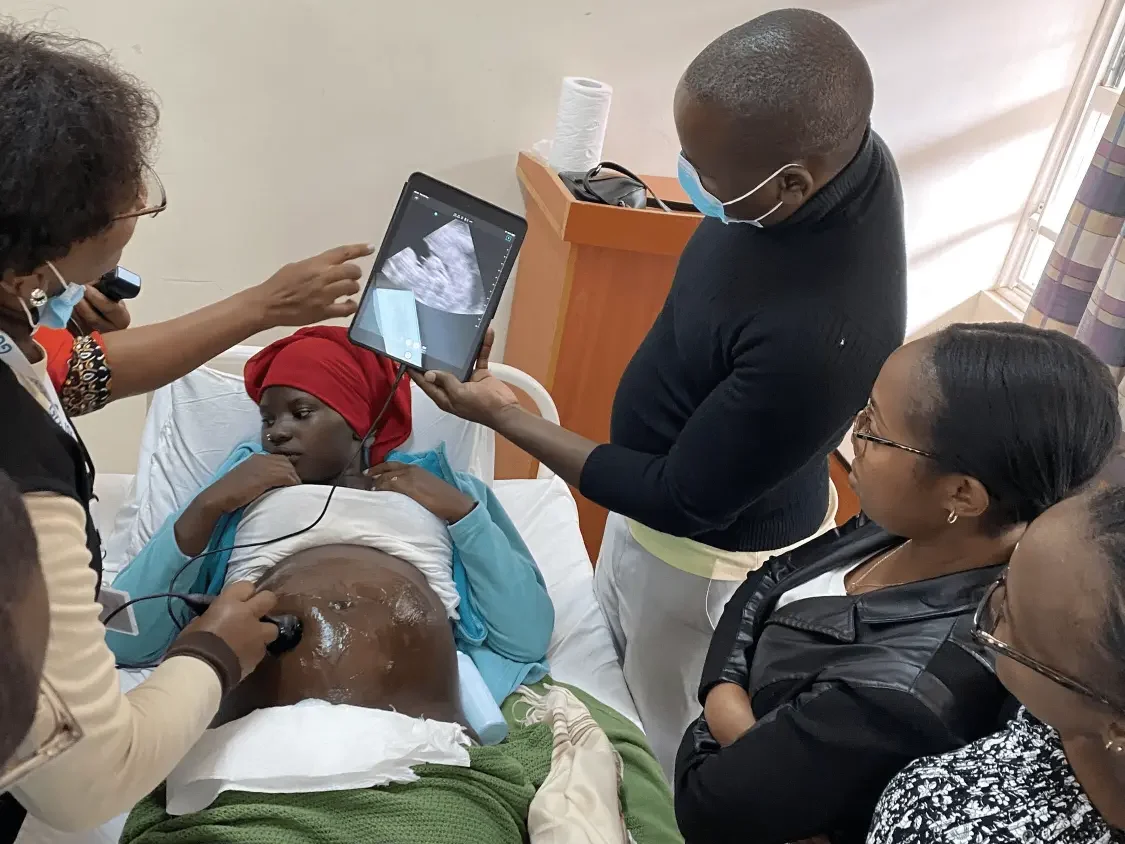
Maternal and Fetal Health: Safer Pregnancies and Deliveries
Perhaps the most dramatic improvements have come in obstetric care. For the first time, many expectant mothers in rural Kenya are getting an ultrasound screening during pregnancy – and the benefits are life-changing. Midwife Jane Waire, who started offering ultrasound in her clinic in 2023, explained that before, “there were things we could not evaluate at all, such as where the placenta is located… Now, with the ultrasound, we can be 100% sure. We can make a quick diagnosis before it’s too late.”[34]. That confidence means that if a baby is in a breech position or the placenta is blocking the birth canal (placenta previa), the mother can be referred to a higher-level facility ahead of time for a safe delivery by C-section, rather than facing an emergency during labor. POCUS essentially gives these midwives “eyes inside the womb”, augmenting their hands and stethoscopes.
Real-world data from the project underscores these benefits:
- In one district, after introducing portable ultrasound, a clinic went six months without a single fetal death, where previously such losses were sadly more common[35]. The midwives credit ultrasound for detecting warning signs early, allowing timely interventions.
- Across Kenya, midwives trained in POCUS have been identifying high-risk conditions at an astonishing rate. A survey six months post-training found about 90% of providers had detected a high-risk obstetric condition (like multiple pregnancy or low fluid) using their Butterfly iQ+ device[36][37]. Many of these conditions would have been missed on physical exam alone. Each flagging of a risk triggers a referral or closer monitoring, potentially averting a tragedy. For example, one midwife discovered that a mother who thought she was carrying one baby was actually carrying triplets – an extremely high-risk pregnancy for a small clinic to manage[38]. Thanks to the scan, that mother was referred to a hospital early, likely saving lives.
- By empowering providers to act early, POCUS is improving maternal and neonatal outcomes. It’s difficult to measure lives saved, but historical comparisons give a hint: as noted earlier, introducing ultrasound in similar contexts has been linked to a 20% reduction in fetal deaths[5]. And beyond survival, there are quality-of-care improvements – mothers experience less uncertainty and anxiety. Seeing their baby on the screen often motivates them to attend follow-up visits[39], and they better understand advice when they can visualize the issue (e.g. a low-lying placenta). This boosts antenatal care attendance and engagement, a crucial factor in healthy pregnancies.
- The ripple effects on healthcare systems are notable. Early findings from Kenyatta University’s evaluation indicate that referrals for obstetric complications are now more appropriate – meaning clinics are referring the right patients at the right time. Unnecessary referrals (which burden families and hospitals) are avoided, while necessary ones happen sooner. Referral patterns have improved, and the proportion of women receiving an ultrasound before 24 weeks (as recommended by WHO) has increased markedly in the project areas[36][40].
All these gains contribute to Kenya’s progress toward safer motherhood. As Butterfly Network reported, by early 2025 the Kenya program alone had facilitated over 500,000 ultrasound scans among 514 practitioners, and this led to countless instances of clinical action – from identifying breech presentations to confirming fetal heartbeat in prenatal check-ups[41][42]. Frontline workers themselves report that POCUS has “given them greater confidence in decision-making and patient management”, and that it often replaces more cumbersome procedures (some midwives have gladly retired the old fetoscope device in favor of using the ultrasound to check fetal heart rate)[43][44]. The use of ScanOne and ScanHub underpins these successes by ensuring that midwives are not operating in isolation – they have a safety net of expert support for interpreting what they see.
Beyond Obstetrics: Building Capacity in General Healthcare
While a major emphasis has been on maternal-fetal health, the POCUS tools are also strengthening broader healthcare delivery in Kenya. The AMPATH program, for instance, is targeting three priority areas: obstetrics, heart failure, and breast cancer screening[45]. These were chosen because they represent common health challenges where early diagnosis makes a huge difference:
- Cardiac Ultrasound: Many patients in Kenya suffer from heart failure or fluid overload related to conditions like hypertension, diabetes, or anemia. In rural clinics, confirming heart failure used to be guesswork – there was no X-ray or echocardiogram available. Now, with a handheld ultrasound, clinicians can perform a quick scan of the heart and lungs. They can check if the heart’s chambers are enlarged or if fluid is backing up in the lungs. “POCUS enables healthcare workers to visualize and diagnose conditions such as heart failure earlier and improves the chances for better treatment and survival,” says Dr. Hussein Elias of Moi University, one of the lead physicians on the project[46]. For a patient with shortness of breath, this means on-the-spot differentiation between, say, pneumonia versus heart failure versus a large pleural effusion – distinctions that would be challenging by stethoscope alone. Early heart failure detection allows prompt initiation of medications and counseling on diet and fluid management, potentially preventing hospitalizations or worse.
- Breast Health: Sub-Saharan Africa faces a rising burden of breast cancer, often detected very late. Mid-level providers rarely had tools to evaluate a breast lump aside from touch. With portable ultrasound, a clinician can scan a palpable breast lump to characterize it (seeing if it’s solid or cystic, measuring its size) and identify suspicious features that need referral for biopsy. This is bringing a form of imaging triage to clinics that never had it. As Dr. Elias noted, POCUS can help catch a “suspicious mass in the breast” earlier[46]. While an ultrasound cannot definitively diagnose cancer, it strengthens the referral system: women with concerning findings can be fast-tracked to get mammography or surgical consultation, whereas simple benign cysts might be managed conservatively. Over time, this could contribute to down-staging breast cancer diagnoses (finding them at stage I/II instead of stage III/IV), which is key to improving survival rates in Kenya[47].
- General Medicine and Trauma: Although not the primary focus of the Kenya projects, it’s worth noting that the same POCUS devices and skills can be leveraged for many other uses. Healthcare workers trained on ScanHub often continue to learn new applications through GUSI’s online modules and the SageAI assistant. They can perform FAST scans for internal bleeding in trauma, assess dehydration in children via ultrasound of the inferior vena cava, guide needle procedures safely, and much more. The projects have essentially created POCUS champions in each facility who often become the go-to people for any ultrasound exam. This elevates the overall diagnostic capability of the facility. As Dr. Mena Ramos of GUSI highlighted, POCUS is “revolutionizing medicine by making it easier, faster, safer and more cost-effective to scan and diagnose patients wherever they are”[21]. That holds true not just for OB, but for virtually every field of medicine in these communities.
Finally, the data tracking built into ScanHub provides tangible evidence of impact that can convince policymakers and donors to sustain and expand these efforts. The platform captures metrics like number of scans, types of findings, and clinical actions taken. For example, by late 2023, GUSI reported that nearly 120,000 scans had been conducted as part of the Kenya maternal health program[48]. As of early 2025, Butterfly Network’s data (from device usage logs) showed over 927,000 minutes of scanning time logged in Kenya, with an average scan taking under 2 minutes as clinicians became more proficient[41][49]. Each of those minutes could mean a life saved or a complication averted. Such data will inform Kenya’s Ministry of Health as it considers national POCUS guidelines. In fact, the results from these projects will guide a planned nationwide rollout of POCUS in Kenya and other low-resource settings in the coming years[50]. This indicates just how successful the model has been – it’s now a blueprint for scaling diagnostics in similar environments globally.
Challenges and Looking Ahead
Implementing a high-tech solution in low-resource settings is not without challenges, of course. The Kenyan teams have navigated issues like software updates and device maintenance (some clinics had brief hiccups when the Butterfly app required an update – now mitigated by providing offline-compatible versions and training on how to update apps[51]). They’ve addressed shortages of ultrasound gel by finding locally available substitutes and improving supply chains[51]. Connectivity can be spotty in remote areas, so ScanOne is designed to store images offline and sync when back online; mentorship feedback might sometimes be delayed by a day or two if internet is weak, but it does get through. There’s also the human factor – some health workers initially felt intimidated by ultrasound technology. Yet, as Dr. Grace Githemo (the Kenyatta University researcher) observed, “the midwives are very motivated” to use it, and even those hesitant at first became enthusiastic when they saw the difference it made for patients[52][6].
Crucially, all partners recognize that ongoing training and support is the linchpin of sustainability. The initial excitement must be followed by continuous learning opportunities. GUSI’s platform is evolving to meet this need – for example, the upcoming ScanVault feature will create a repository of “best scans” and case studies from the field, so Kenyan providers can learn from each other’s cases. The SageAI tool is expected to gain new capabilities in image analysis (imagine an AI that can auto-measure a fetus or flag an abnormal heart chamber, giving providers instant feedback even before a human mentor looks). These innovations will further enhance the self-reliance of clinicians using POCUS.
Policy support is also growing. With evidence from AMPATH and Kenyatta University, the Kenyan government is increasingly supportive of POCUS. We may soon see national guidelines integrating ultrasound into standard antenatal protocols and primary care algorithms. The ultimate vision is that every pregnant woman in Kenya receives at least one ultrasound during pregnancy (per WHO recommendations)[40][53], and that any patient with an acute condition can be assessed with POCUS at their first point of contact. Achieving this at scale will require thousands more devices and trained personnel, but the blueprint is now proven.
For donors and global health supporters, the Kenya POCUS initiative offers a compelling case study of impact. A relatively modest investment – a handheld device and some training – at a peripheral health center can yield outsized benefits: lives of mothers and babies saved, serious illnesses caught earlier, referrals optimized, and healthcare workers empowered with new skills. And it does so cost-effectively. Preliminary analyses suggest that the cost per ultrasound scan in these programs is just a few dollars (or less) when accounting for the volume of patients served[54][55]. The Butterfly devices cost a fraction of traditional ultrasound machines, and training in bulk leverages economies of scale. In Kenya, GUSI estimated an average cost of only around $0.20 per scan in one Gates-funded program (after the initial investment)[56] – an incredibly low figure for such a high-impact intervention.
Conclusion: A New Era of Accessible Imaging
The journey of ScanOne and ScanHub in Kenya illustrates how technology and collaboration can transform healthcare in even the most resource-constrained settings. What was once the domain of specialists in big hospitals – ultrasound imaging – is now being put into the hands of nurses in village clinics, with outcomes that are nothing short of remarkable. A midwife who could only rely on her fingertips and fetoscope can now literally see inside a patient, and with that insight, take timely action to save lives. And she’s not alone; through ScanHub, she’s connected to a community of experts and peers, continuously learning and improving.
As one Kenyan nurse-sonographer put it, “We know that accurate, timely diagnosis correlates to good clinical outcomes. Wherever POCUS is used… it will help improve outcomes.”[32] The experiences in Kenya bear this out: from mothers who safely delivered because risks were spotted early, to chronically ill patients who got the right treatment faster, the impact is being felt family by family.
Importantly, this is a story of empowerment. The local clinicians are not just end-users of a donated gadget; they are becoming leaders in their communities for ultrasound-based care. Programs like AMPATH’s ensure that capacity is built locally – Kenyan doctors, nurses, and midwives training one another, supported by global partners but ultimately in charge of their own healthcare innovation. ScanOne and ScanHub, backed by the philanthropic and technical support of entities like the Gates Foundation and Butterfly Network, have simply been the catalysts.
Moving forward, the hope is to expand such models throughout Kenya and replicate them in other countries. Already, GUSI’s global health arm has projects in Ghana, South Africa, Malawi, and beyond, adapting the lessons learned in Kenya to new contexts[57][58]. The convergence of cheap portable ultrasound hardware, cloud-based software (for mentorship and data), and committed partnerships is shifting the paradigm of diagnostics in global health.
In Kenya, one can truly say the ultrasound revolution has arrived: it’s in the hands of the people who need it most, supported by ScanOne, ScanHub, and a network of champions. And as the data keeps showing lives saved and conditions detected, we are likely witnessing the beginning of a new era where no clinician has to say, “We have to figure it out without tools,” and no patient has to travel hours for a scan – because the scan, and an expert’s advice, are available on the spot. “POCUS is a game changer,” Dr. Ramos of GUSI said[22]. In the villages and towns of Kenya, that game is changing for the better, one scan at a time, with ScanOne and ScanHub lighting the way.
Sources:
- AMPATH Kenya News – Point of Care Ultrasound Education and Care Integration in Western Kenya[11][12][46][59]
- Global Ultrasound Institute – Global Health Initiatives (GUSI Global Health program description)[10][54]
- Global Ultrasound Institute – ScanOne Mobile App description[7]
- Gates Foundation – Caring for Mothers with Ultrasounds, AI, and Nurse Midwives (Gates Foundation article)[5][6][35]
- Butterfly Network – Case Study: 1,000 POCUS Probes in Kenya and South Africa[37][42]
- AlignMNH (Heather H. Donahoe) – Transforming Maternal and Neonatal Health through Portable Ultrasound[25][36]
- PR Newswire (GUSI) – Historic Ultrasound Training Initiative in Africa[26][21][32][22]
- PR Newswire (GUSI) – Training initiative results[48].
[1] [11] [12] [13] [29] [33] [45] [46] [47] [50] [59] AMPATH Leads Point of Care Ultrasound Education and Care Integration in Western Kenya — AMPATH Kenya
[2] [5] [6] [9] [19] [20] [34] [35] [38] [39] [51] [52] Caring for Mothers with Ultrasounds, AI, and Nurse Midwives
[3] [4] [21] [22] [23] [24] [26] [27] [32] [48] Global Ultrasound Institute Completes Historic Ultrasound Training Initiative To Reduce Maternal and Neonatal Deaths in Africa
[7] scanOne for Android – Free App Download
[8] Newsletters – Global Ultrasound Institute
[10] [14] [15] [54] [55] [56] [57] Global Health Initiatives – Global Ultrasound Institute
[16] [25] [28] [36] [40] [53] [58] Transforming Maternal and Neonatal Health through Deployment of Portable Ultrasound at Scale – AlignMNH
[17] [18] [30] [31] [37] [41] [42] [43] [44] [49] Butterfly deploys 1,000 POCUS probes to practitioners across Kenya and South Africa


